U1355 – RAMO-IT -
Molecular Radiotherapy and Therapeutic Innovations
Transforming radiotherapy: toward precision medicine
Unit U1355/RAMO-IT (formerly “U1030”) develops an integrated research program aimed at profoundly transforming the use of radiotherapy in oncology. Historically based on standardized approaches, radiotherapy now faces major limitations related to the biological heterogeneity of tumors, variability in patient responses, and the occurrence of sometimes debilitating toxicities.
In this context, the unit proposes an ambitious paradigm shift: moving from a “one-size-fits-all” approach to precision radiotherapy, personalized, biologically informed, and aligned with the need for global harmonization of practices.
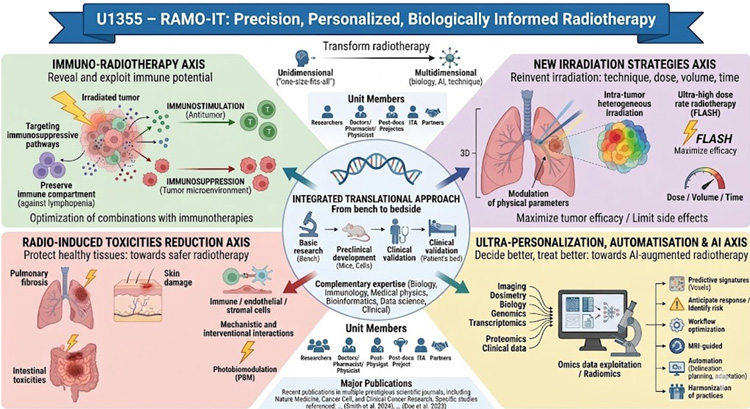
Immuno-Radiotherapy Axis
Revealing and harnessing the immune potential of radiotherapy
At the core of this strategy lies immuno-radiotherapy, a structuring axis of the unit’s work. Radiotherapy is now recognized as a powerful modulator of the immune system, capable of both stimulating antitumor responses and inducing immunosuppressive mechanisms. Research conducted at U1355 aims to decipher these complex interactions within the tumor microenvironment and to steer this balance toward effective immunity.
This includes identifying and targeting irradiation-induced immunosuppressive pathways, as well as optimizing combinations with immunotherapies. Particular attention is given to radiation-induced lymphopenia, now recognized as a major determinant of treatment response, opening the way to new planning strategies aimed at preserving the immune compartment.
New Irradiation Strategies Axis
Reinventing irradiation: technique, dose, volume, and time as therapeutic levers
In parallel, the unit explores innovative irradiation strategies by systematically investigating the physical parameters that determine biological response. Research focuses on modulation of dose, volume, and dose rate, with the goal of maximizing tumor efficacy while minimizing side effects.
Emerging approaches such as heterogeneous intra-tumoral irradiation or ultra-high dose-rate radiotherapy (“FLASH”) are studied in an integrated manner, combining precise physical analyses with in-depth biological characterization. These studies contribute to redefining treatment standards on rational and mechanistic grounds.
Axis: Reduction of Radiation-Induced Toxicities
Protecting healthy tissues: toward safer radiotherapy
Reducing radiation-induced toxicities is another key pillar of the program. The unit develops mechanistic and interventional approaches to prevent or mitigate the deleterious effects of radiotherapy on healthy tissues.
This work spans a wide range of organs and complications, including lung fibrosis, skin and mucosal damage, intestinal toxicities, and neurocognitive effects. It is based on a detailed understanding of interactions between immune, endothelial, and stromal cells, and leads to concrete therapeutic innovations, some of which are already under clinical development. Among these approaches, photobiomodulation (PBM) is being explored as a promising modality to limit radiotherapy-related toxicities.

Axis: Ultra-personalization, Automation & AI
Better decisions, better treatments: toward AI-augmented radiotherapy
Finally, Unit U1355 is fully engaged in personalized medicine through the development of approaches based on artificial intelligence, radiomics, and more broadly, omics data integration. By combining imaging, dosimetry, molecular biology, genomics, transcriptomics, proteomics, and clinical data, researchers develop predictive signatures to anticipate treatment response, identify patients at risk of relapse, and guide therapeutic decisions at a fine scale, down to the voxel level.
Beyond prediction, these approaches also transform clinical practice by optimizing radiotherapy workflows, with a key role for MRI in guiding and refining each step. The unit develops tools to automate complex and time-consuming tasks, particularly contouring, treatment planning, and daily adaptive therapy, to support radiation oncologists in decision-making and improve treatment reproducibility.
In this perspective, the work also contributes to harmonizing practices across centers by providing robust, standardized, and transferable solutions, promoting precision medicine accessible on a broader scale.
This multi-scale and multi-level integration (from voxel to care pathway) paves the way for individualized treatment adaptation, aligned with the specific characteristics of each tumor, each patient, and clinical environments.

Axis: Integrated Translational Approach
From bench to bedside: an integrated translational research framework
All of this work is embedded in a strongly translational approach, based on a close continuum between fundamental research, preclinical development, and clinical validation. This organization fosters constant back-and-forth between the laboratory and the patient bedside, accelerating the transfer of innovations into clinical practice.
Highly interdisciplinary, the unit relies on complementary expertise in biology, immunology, medical physics, bioinformatics, data science, and clinical practice, as well as a high-level network of academic and industrial collaborations.
