CD8 T-cell immunity and immunotherapy in lung cancer
This group belongs to the UMR 1186 - Integrative tumor immunology and immunotherapy
Despite advances in immunotherapy, a large fraction of cancer patients fails to respond. Immune mechanisms behind this resistance are poorly elucidated. The objective of our research program is to comprehensively characterize and study the role of a new class of white blood cells, called resident memory T cells (TRM), in antitumor immunity and response to cancer immunotherapy.
Research topics
Our team highlighted several constitutive elements of the tumor microenvironment (TME) involved in the regulation of antitumor T-cell response, in particular the influence of TGF-β on the expression and signaling of CD103 in CD8+ tumor-resident memory T cells (TRM), and the role of this integrin to sustain specific cytotoxicity and promote T-cell recruitment within epithelial tumor regions. Our objective is to make new advances in the field of TRM cells and tumor resistance to T-cell-mediated cytotoxicity and immune checkpoint blockade immunotherapy, such as anti-PD-1. Our program aims at:
1) characterizing tumor CD4+ TRM and determining their role in regulating antitumor T-cell immunity and response to anti-PD-1 using human lung cancer and mouse tumor models;
2) developing an air-liquid interface (ALI) culture system to study the cross-talks between lung cancer cells and immune cells, in particular cytotoxic T lymphocytes, and their consequences on both cell types;
3) defining a composite immune signature predictive of clinical response to anti-PD-1 by assessing the involvement of TRM, antigen-presenting machinery (APM) in tumors and T-cell neoepitopes;
4) studying the role of neuropilin (Nrp)-1 in regulating CD4+ effector T-cell functions and antitumor immune response and
5) providing a proof of concept of a combination immunotherapy based on the preprocalcitonin (ppCT) peptide vaccine and anti-PD-1 in preclinical humanized mouse models. This last research axis has led to the foundation of a startup, ElyssaMed. Through its various aspects, the aim of our program is to better understand how the TME influences the behavior and functions of effector T cells, in particular TRM, and impacts response to immunotherapies. Our goal is to improve current cancer treatments and contribute to the development of more effective combination therapies. To do so, we have established solid interaction with clinicians from Gustave Roussy and have access to all Gustave Roussy’s platforms. Our unit belongs to several research networks, is attractive for post-doc and young scientists, and has established numerous national and international collaborations.
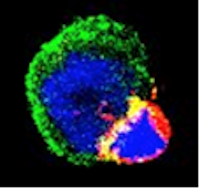
An immune synapse between a CD103+CD8+ TRM cell freshly isolated from human lung tumor-infiltrating lymphocytes and a cognate tumor target cell
